Free Pulmonary Course on Reading Pulmonary Function Tests
by Joshua Benditt, MD
What Are Pulmonary Function Tests Used For?
Pulmonary function testing provides a method for objectively assessing the function of the respiratory system. The tests do not always diagnose specific conditions but should be used to gain a greater understanding of a patients' clinical problem. Questions which may be answered with pulmonary function tests include:
- Identification of certain primary diseases of the respiratory system.
- Following the course of a specific disease over time.
- Quantitation of the severity of disease.
- Assessment of a response of a disease process to treatment.
- Exclusion of certain disease processes from diagnostic consideration (e.g. upper airway obstruction).
Pulmonary function tests must always be analyzed within the context of the patient being tested. Age, height, weight, race, and sex directly affect the results which one would predict for a given individual. Diseases which the patient may have or drugs which they are taking may be important in the interpretation of the patient's test. For instance, in a patient taking gold shots for rheumatoid arthritis, the finding of a restrictive PFTs, particularly if they are new, is very significant. Thus, the clinical context is extremely important in both understanding and interpreting PFTs.
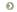 Top of Page Top of Page
What Types of Measurements Can Be Made In Pulmonary Function Testing
There are essentially four categories of information which can be obtained with routine pulmonary function testing:
- Lung volumes which can allow us to measure the maximum volume of the lungs as well as sub-compartments thereof.
- Flow rates which measure the maximal flow of gas out of (and sometimes into) the lung.
- Diffusing capacity which measures the transfer of gas from the alveolar space into the capillary blood stream.
- Maximal inspiratory and expiratory pressures which measure the applied strength of the respiratory muscles.
Prior to examining how each of the measurements are made, let us examine some of the volumes and flow rates which we will be using in our evaluation of PFTs. Although the lung volumes can be divided into a large number of compartments including volumes and capacities (which are the combination of two or more volumes), there are four important volumes which should be remembered:
- total lung capacity (TLC) or the total volume of gas contained in the lungs;
- functional residual capacity (FRC) or the volume of gas left in the lungs with the individual relaxed at the end of expiration;
- residual volume (RV) the volume of gas left in the lungs at the end of forced expiration; and
- vital capacity (VC) the difference between the largest (TLC) and the smallest (RV) lung volumes which can be obtained. These volumes are shown in Figure 1.
Fig 1
Measurements of Lung Volumes
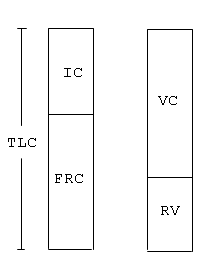
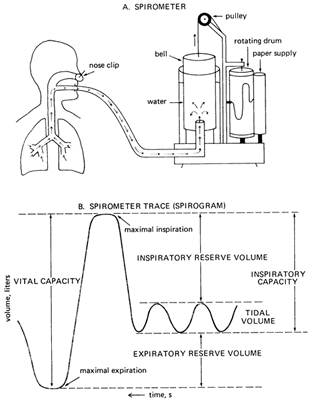
Measurement of some of the volumes such as vital capacity is easy and can be performed with the simple spirogram. By having the patient breath to their maximal capacity (TLC) lung capacity and blow out as far as possible (RV), the vital capacity can be recorded (see Figure 2 below).
Fig 2
Other volumes such as residual volume (RV) and total lung capacity (TLC) cannot be measured with the spirometer but require an additional measurement technique, either the body plethysmograph or helium dilution in order to be determined. This is because the amount of gas left in the thorax at maximal expiration (RV) cannot be measured by the spirometer. By using one of the other techniques, we can determine this volume and subsequently all other volumes and capacities including TLC. (The body plethysmograph and helium dilution techniques are shown in Fig 3a below).
Fig 3a
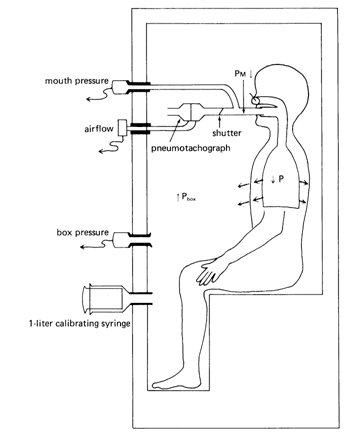
Pbox x Vbox = Pbox f x (Vbox i -∆V)
Once 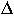 V has been solved for we can then go on to solve for the thoracic gas volume in the following equation: V has been solved for we can then go on to solve for the thoracic gas volume in the following equation:
PMi x VLi = PMf x (VLi + ∆V)
This equation follows from the Boyle's Law and tells us that the initial pressure measured at the mouth (PMi) times the lung volume at which that pressure is measured (VLi) will be equal to the new mouth pressure (PMf) x the new lung volume (VLi + ∆V) while the patient is making small changes in their lung volume by panting against the closed shutter.
Fig 3b
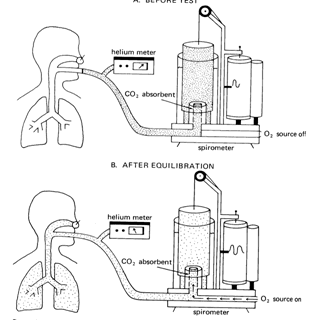
The helium-dilution technique makes use of the following relationship: If the total amount of substance dissolved in a volume is known and its concentration can be measured, the volume in which it is dissolved can be determined.
Amount of solute = concentration of solute x volume of solvent
In the helium-dilution technique, helium is inspired and dissolved in the gas in the lungs. The concentration of helium is determined with a helium meter. allowing calculation of the patient lung volume. Helium is used for this test because it is not taken up by the pulmonary capillary blood. The total amount of helium does not change during the test. The helium concentration is monitored continuously with a helium meter until its concentration in the inspired air equals its concentration in the subject's expired air. At that point the concentration of helium is uniform in the spirometer and the patient's lung.
The test is stopped at the end of a normal tidal volume, FRC and the volume of FRC is calculated:
Initial Concentration of helium x Initial Spirometer Volume =
Final Concentration of Helium x (Final Spirometer Volume + FRC)
Fhei x Vsp = Fhef (Vspf + VLf)
 Top of Page Top of Page
Next: What determines
the major lung volumes?
|