What Determines the Major Lung Volumes?
Total lung capacity is determined by the ability of the inspiratory
pump (brain, nerves, muscle) to expand the chest wall and lungs which have
a strong tendency to recoil inwards at high lung volumes. Any
breakdown in the ability of pump to function will result in a smaller
total lung capacity (restrictive lung disease). Neuromuscular
disease is an example of this. Diseases which increase inward recoil
of the lung (pulmonary fibrosis) will lead to a smaller TLC.
Diseases which lead to a reduction in inward recoil of the lung
(emphysema) result in an increase in TLC known as hyperinflation.
Residual volume (RV) is determined in healthy younger individuals by
the competition between the strength of the expiratory muscles and
compressibility of the chest wall. However, by the onset of middle
age or in obstructive lung disease RV appears to be determined by a "flow
limitation"; expiratory flow rates at low lung volumes are so low
that expiration is prolonged and is not completed down to the original RV
by the time the subject gives up the effort and takes another breath.
Vital capacity (VC) is determined by the difference between TLC and RV
and changes with variations in RV or TLC. It is easily measured and
reliable and can check the measured validity of a measured change in RV or
TLC. FRC is the relaxation volume at the end of expiration. It
is not a reliable measurement and requires excellent cooperation on the
part of the subject. In patients with obstructive lung disease FRC
may be elevated. This imposes a significant extra load on the
inspiratory muscles which can results in muscle fatigue.
 Top
of Page
Top
of Page
What Determines Airflow Through the Bronchial System?
Air flows through a tube if there is a pressure difference between the
ends. In the respiratory system the pressure difference is between
the alveolar pressure and the pressure at the airway opening or mouth.
Flow may be laminar (smooth) or turbulent dependent on characteristics of
the gas and the tube through which it is traveling. Most of the
resistance to airflow occurs in the first few divisions of the airways.
The more distal airway divisions, because of their large cross-sectional
area, constitute a silent zone of airway resistance.
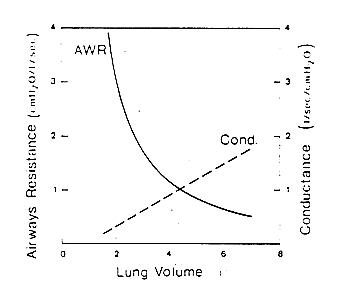
Resistance to flow is not constant at all lung volumes. As the
lung expands, airways enlarge reducing the airways resistance at high lung
volumes. Airways resistance increases at lower lung volumes. A
plot of airways resistance vs. lung volume is shown in Fig 4.
Fig 4
 Top
of Page
Top
of Page
Other factors besides lung volume can affect airway resistance.
Smooth muscle within the wall of the same bronchi can contract and
increase airways resistance. Secretions in airways or edema in the
airway wall can also increase airways resistance. In patients with
emphysema, loss of tethering of small airways open during exhalation leads
to collapse and an increase in resistance to airflow. All
obstructive lung diseases are characterized by an increase in resistance
to expiratory flow.
Measurement of Expiratory Flows
Measurement of expiratory flow is extremely useful to us particularly
in identifying obstructive lung disease but in a number of other ways
also. Expiratory flows are measured during the forced expiratory
spirogram (Figure 2). Again, the patient breaths
to TLC and forcefully exhales to residual volume generating the expiratory
spirogram with volume plotted against time.
The spirogram can be broken up into subdivisions. The ones
which we are most concerned about are
- the FVC which has been mentioned previously and represents the
entire volume exhaled from the lungs in a forced breath,
- the FEV1 or the volume of gas exhaled in the first one
second of exhalation,
- the FEF25-75 which is the flow of gas exhaled during the middle
half of the vital capacity previously known as the maximal mid
expiratory flow or (MMFR).
The forced expiratory maneuver has been called "an unnatural act"
because it is rarely if ever performed during daily activities.
Nevertheless, it probes a very important pathophysiologic limit.
Beyond a modest expiratory effort, the limit to flow is
effort-independent; pushing harder does absolutely no good. The
limit, however, is markedly volume dependent ranging in healthy persons
from 10 liters per second at high lung volumes to near zero flow at RV.
The limit is lowered at all lung volumes by primary narrowing of airways
or narrowing due to decrease in lung recoil (emphysema) and is responsible
for the ventilatory impairment seen in these obstructive lung diseases.
 Top
of Page
Top
of Page
Flow Volume Loop Analysis
In addition to portraying the spirogram as volume plotted against
time, it can also be plotted as flow against volume as shown below in
figure 5. This can be particularly helpful in identifying
obstruction lesions of the upper airway.
Fig 5
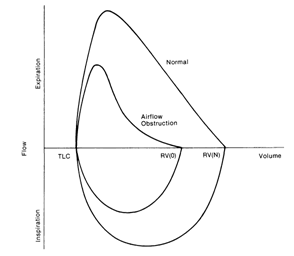
Fig 6: Intra and
extrathoracic large airway obstructing lesions
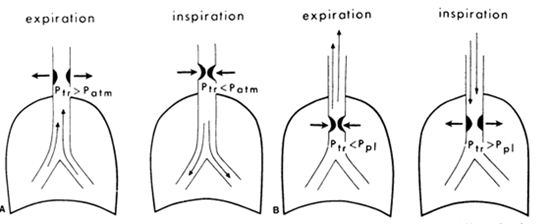
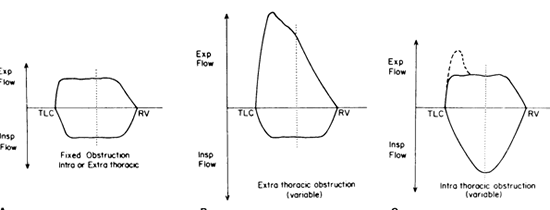
Fig 7: Flow-volume loops
in intra and extrathoracic lesions
Diffusing Capacity
The diffusing capacity is a measure of the transport of gas across the
alveolo-capillary membrane. The techniques of this measurement is
discussed will be discussed with you. The diffusing capacity reflects the
surface area of the alveolo-capillary membrane as well as its thickness
and the driving pressure for gas across the membrane. It can be reduced in
diseases such as emphysema, pulmonary fibrosis, or pulmonary vascular
disease. It can also be reduced in patients with anemia.
 Top
of Page
Top
of Page
< Previous: Reading Pulmonary Function Tests | Next:
How To Interpret
Pulmonary Function Tests